More mental health patients sent 'hundreds of miles' for care
- Published

Terry Proudfoot said not being able to see her dog was a barrier to recovery. "I don't feel complete without a dog with me," she said.
More mental health patients are being sent hundreds of miles from home for treatment, new figures have revealed.
NHS figures showed, external more than 3,000 patients were placed over 100km (62 miles) from home for treatment because of a lack of beds - a 35% increase since last year.
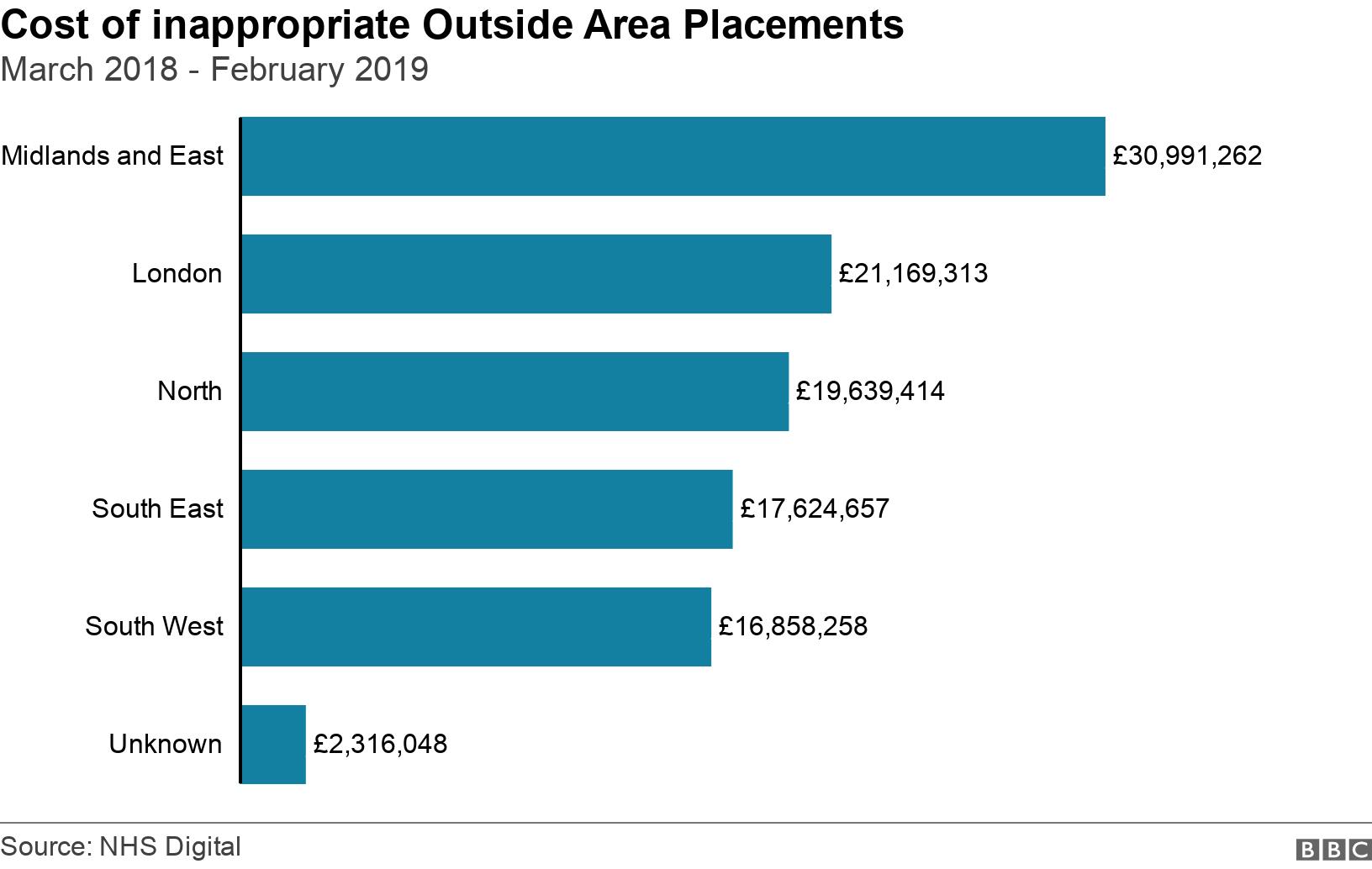
The NHS spends an average of £9m a month on so-called inappropriate Outside Area Placements (OAPs).
The Government has pledged to eliminate inappropriate placements by 2020-21.
Vicki Nash, head of policy and campaigns at the mental health charity Mind, said: "We have heard repeated promises from the NHS to completely eliminate inappropriate out of area placements, and yet we know the number of these placements has increased.
"Too many of us with mental health problems are being forced to travel hours from friends and family to receive the treatment we need.
"This can worsen people's chances of recovery, as well as being expensive for the NHS."

'My entire reality was ripped away'

Hazel Scott estimates she spent more than 250 hours visiting her daughter Katie while she was placed away from home for mental health treatment
A few months before her 18th birthday Katie Scott was sectioned under the Mental Health Act.
She was moved 160 miles (257km) away from her Wokingham home to a hospital in Norwich to continue her treatment for borderline personality disorder and anorexia.
"I remember when I got there lying on my bed for four hours and just crying. I didn't want to eat, I didn't want to move," Ms Scott told the BBC.
"The fact that it was so far away meant that there was probably a four-month delay in my recovery."
"It felt like my entire reality, everything I had known ever known, had been ripped away".
Her mother Hazel made an eight-hour round trip every weekend for seven months to see her daughter.
She said mental health treatment was "woefully underfunded".
"Having young people or adults placed great distances from their home doesn't just impact the patients, it impacts their family massively.
"Your mind goes into overdrive thinking about how she's doing and how she's coping.
"Local mental health care is essential. The more we can have the better it will be."


The NHS has published monthly figures on mental health placements since October 2016 and detailed statistics have been available for two years.
Between March 2018 and February 2019 - the latest period available - the NHS spent £109m on placing mental health patients outside of their local area due to a lack of bed space.
On average 80% of placements were in private mental health care units, funnelling money away from stretched NHS services.
Last year 8,545 inappropriate OAPs were started.
The average placement lasted 27 nights but 255 placements lasted more than three months.
Of the 275 patients moved more than 300km (186 miles) for a bed last year, nearly half were from the South West of England.

A 99% reduction

Terry Proudfoot was one of thousands of patients placed miles from her home for mental health treatment
"All I knew was I was going to be away from home, I didn't actually know where I was going."
Terry Proudfoot has suffered with mental health difficulties throughout her life, which led to bouts of serious self-harm.
In 2010 her condition worsened and she was placed in a hospital in Bradford, 40 miles (64km) from her home and family.
She did not return home for four years, bouncing between two hospitals.
It was during this time Ms Proudfoot's home NHS Trust in Sheffield instituted a "radical" new health programme.
Since 2014 Sheffield Health and Social Care NHS Foundation Trust has offered people with complex mental health needs a home, through the South Yorkshire Housing Association.

Mike Hunter said Sheffield Health and Social Care NHS Foundation Trust installed the LivingWell programme after realising the existing model "had things wrong"
The LivingWell partnership provides the patient with in-home medical care and a key worker to help maintain their property.
"Everyone knows you can't do rehabilitation away from someone's community," Mike Hunter, executive medical director of Sheffield NHS Foundation Trust, told the BBC.
The programme has "drastically improved" mental health outcomes in the area, Mr Hunter said.
"We've achieved a 99% reduction in hospital bed placements for people in severe mental health need," he said.
Since returning home Ms Proudfoot said her mental health had drastically improved.
"You can't really get back to your normal level of function when you're in an unfamiliar institution," she said.
"It's about a sense of belonging.
"I do still get anxious, I do get worried, but it feels more manageable."

A Department of Health and Social Care spokesperson said: "It is completely unacceptable for patients to be sent away from their family and friends for treatment — that is exactly why we've committed to end inappropriate out of area placements by 2020-21.
"We are transforming mental health services with a record spending of £11.98bn in 2017-18 and, as part of our Long Term Plan for the NHS, announced a further expansion of mental health services, with an additional £2.3bn every year in real terms by 2023-24."
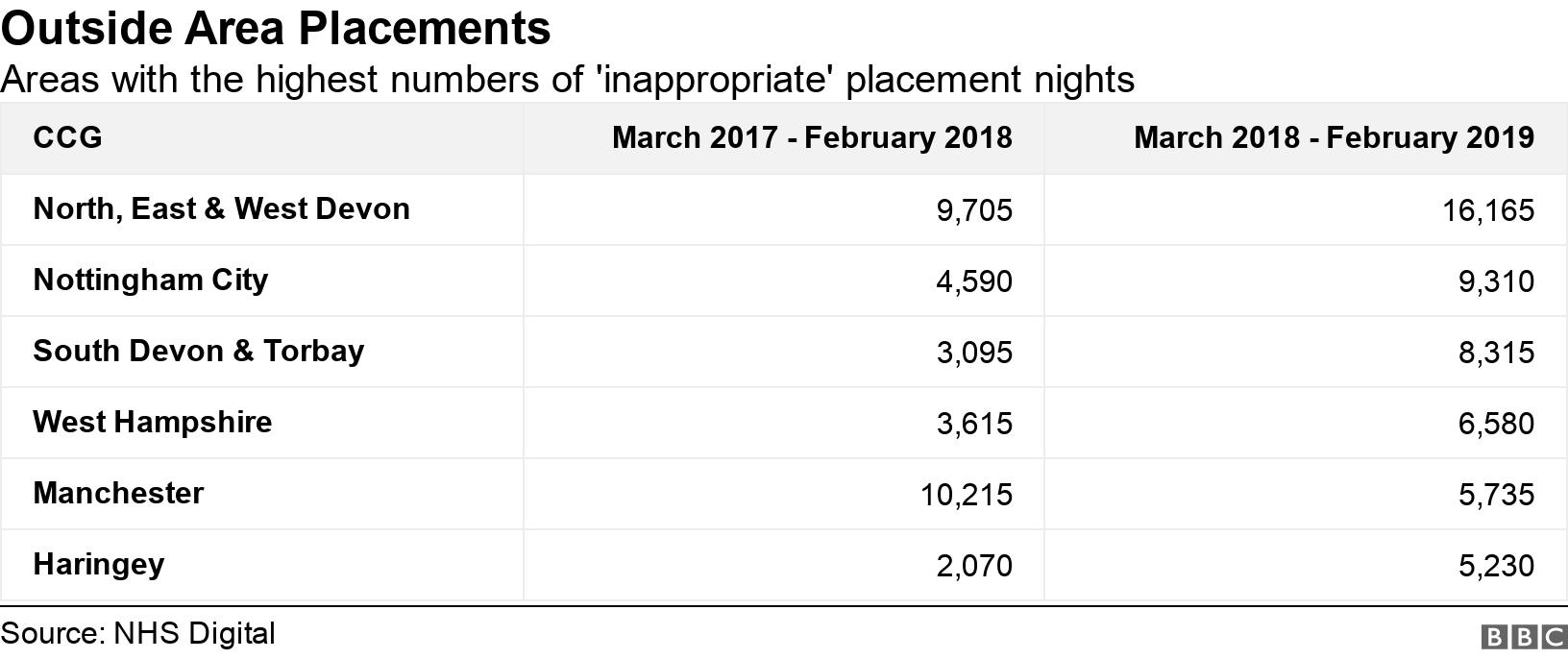
A spokesperson for Northern, Eastern and Western Devon CCG, which had the highest number of inappropriate OAPs last year, said: "We know how hard it can be for people and their families to receive treatment away from their local area and we only ever arrange care outside Devon when it is absolutely necessary.
"We are working closely with our providers to reshape community services so that people can receive care as close to home as possible."
The CCG merged with South Devon and Torbay CCG on 1 April - outside the period covered by the figures.
- Published10 May 2019

- Published15 July 2015

- Published12 May 2017
