A&E nurse: Most challenging I've seen in 30 years
- Published

Susan Beswick's whole nursing career has been at Royal Bolton Hospital
There are 10 patients in the corridor and the nurses are about to go out to assess two more waiting in an ambulance outside.
The senior sister, Susan Beswick, who has worked in the hectic and often stressful world of NHS accident and emergency for 30 years, says she has never seen anything like it.
"The last six to 12 months have been more challenging than I have ever known," she says.
"We have been exceptionally busy for quite a number of weeks now. We're running two to three times above our capacity continually and often more than that."
Susan's whole nursing career has been at Royal Bolton Hospital, which, like many in the country, is facing overwhelming demand from a growing as well as ageing population and has out-of-date buildings that are not fit for purpose.
It is underperforming in the national targets, with lengthening ambulance response times over the past few years.
Trolleys line the corridor leading from the entrance where paramedics bring in patients. Space is running out - and Susan moves quickly between patients, ambulance crews and doctors, assessing the situation.

Staff are working flat out
It is early afternoon and far from unusual - but staff know it always becomes busier as the evening approaches.
At times, doctors and nurses are having to go out to ambulances to assess and treat patients, because there is no room in the department.
In the corridor, a nurse sits next to an elderly woman who seems to have come in after a fall, reassuring her.
Royal Bolton is trying everything possible to manage and speed up the flow through the emergency department.
Patients are triaged, with some being sent to a rapid-assessment unit and the less seriously ill to a minor-injuries unit or an urgent-care centre with GPs on hand, following standard best practice at major hospitals.

Susan works closely with ambulance crews to ensure patients are seen as swiftly as possible
A policy of cohorting, adopted by many hospitals, has been agreed between emergency-department staff and paramedics. One member of an ambulance team will be left to look after two or three patients in a corridor, allowing others to get back on the road more quickly.
The problem is space. There are simply too many patients coming in to be accommodated, even with all the streaming initiatives.
The buildings have not been expanded in recent years - but there has been a 50% increase in the number of ambulances arriving compared with pre-pandemic levels, sometimes 60 a day.
Before Covid, 300 a day were coming into the emergency department - but in the past few days, it has been nearly 500.
Move rapidly
In the "majors" area, where the sickest patients are seen and cared for, there is a constant buzz of noise.
Doctors, nurses and healthcare assistants huddle around screens, checking on priorities and data on the patients coming in.

Patients were lined up in the corridor
They move rapidly to cubicles to look at the most urgent cases. Even here, some patients have to be fitted in, sitting on chairs tucked in among work stations.
"It's not very private for the patients," Susan says. "We are having to nurse them on a corridor that's a thoroughfare - it has continually got personnel, patients and ambulances crews passing by all the time."
She knows the situation is far from ideal and very different from what was normal earlier in her career.
"We are providing the best care in the safest way that we can do," Susan says. "It certainly isn't the best and safest care that we would like to give."
'Managing pressures'
Flu and Covid have added to the pressures on the hospital.
Respiratory-department head Dr Rizwan Ahmed says it is now tougher than during the worst of the pandemic.
"We feel staff are exhausted," he says. "We have used all our resources and it is more difficult than during Covid because then a lot of services were stopped - but now, we are keeping on all elective services and managing pressures at the front end."
Diane O'Rourke has been seriously ill with flu but is recovering and grateful to the staff.
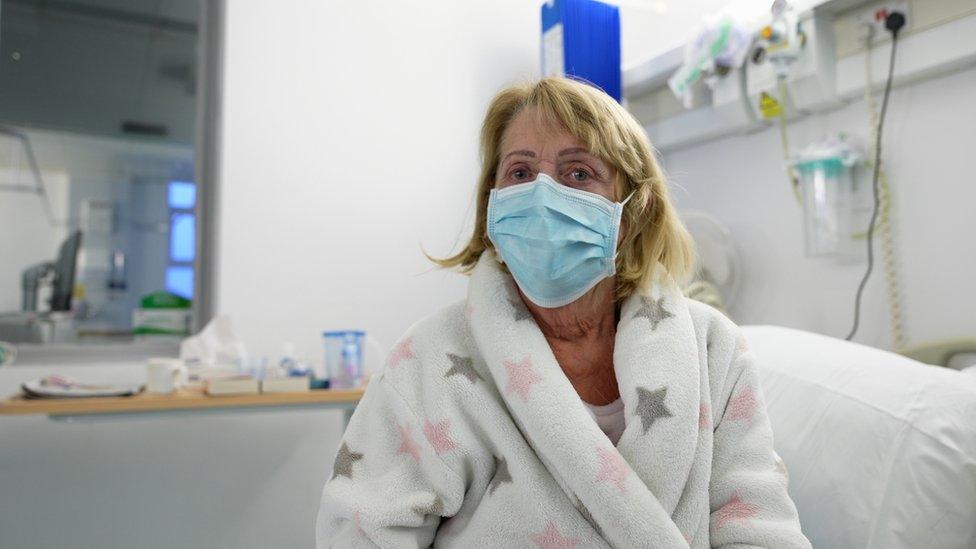
Diane was driven to A&E by her husband
She did not have to wait long in the emergency department - because doctors realised the gravity of her condition - but she only got there because of quick thinking by her local GP.
Diane's husband took her to the local surgery and was told to drive her immediately to hospital, as an ambulance wait would be too long.
"I couldn't walk," she says. "He had to carry me in. He was holding me. The GP saw me and straight away she got me sorted. Once she saw me, she knew I was ill. She typed a note out and sent me straight to A&E. I'd say that the GP saved my life."
Flat out
Difficulties finding beds because some medically fit patients cannot be discharged are all too familiar.
Where possible, Royal Bolton's occupational therapists and physios discuss rehabilitation with patients soon after their arrival. They start planning community care to ensure a timely discharge.
There is no doubt conditions are grim in the emergency department. With staff working flat out in buildings designed for a patient flow not seen for at least a decade, Royal Bolton's experience reflects that of most major hospitals.
In December, a record low of 65% of patients going into A&E in England were treated or assessed within the benchmark of four hours. More than 54,000 had to wait more than 12 hours on a trolley or in a chair after a decision to admit.
However much stress and strain the team is under, Susan remains calm and philosophical.
"The workload is tough," she says, "but we all try and support one another to do the job, to adapt and change our ways of working.
"We are A&E nurses and we take what's put in front of us and deal with it the best we can."
